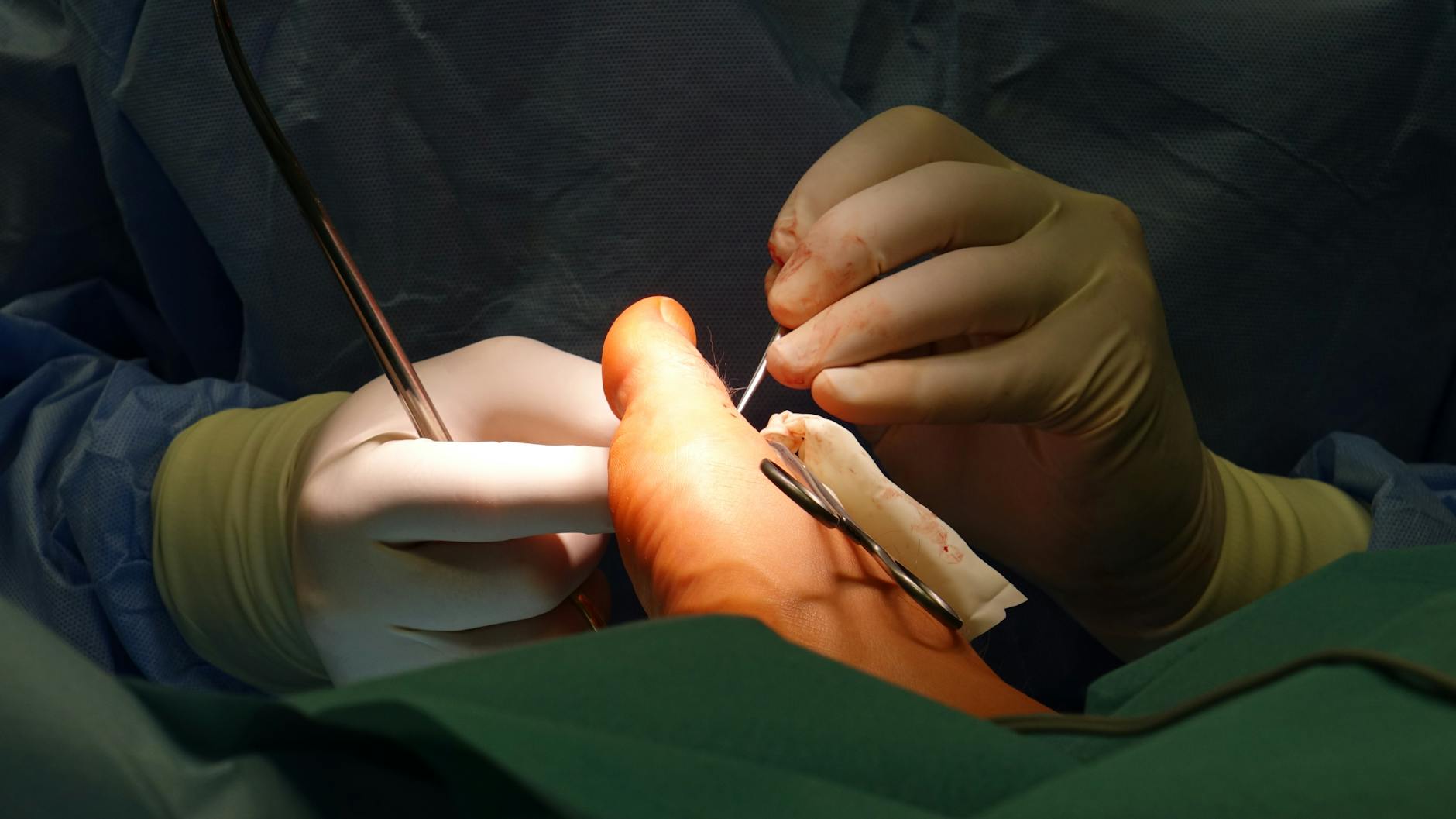
is a critical medical procedure used to treat various blood-related conditions. It involves removing a patient’s blood and replacing it with fresh donor blood or plasma. This process is essential in managing severe cases of jaundice in newborns, sickle cell disease, and other hematological disorders. Understanding the intricacies of exchange transfusion can help patients and caregivers make informed decisions about their healthcare options.
Quick Answer:
- Exchange transfusion replaces a patient’s blood with donor blood.
- Used for conditions like severe jaundice and sickle cell disease.
- Involves careful monitoring and skilled medical professionals.
What Is Exchange Transfusion?
is a medical procedure where a patient’s blood is gradually removed and replaced with donor blood or plasma. This technique is primarily used to treat conditions such as severe neonatal jaundice, sickle cell anemia, and certain types of poisoning. The procedure helps in reducing high levels of bilirubin, removing abnormal red blood cells, and eliminating toxins from the bloodstream.
Why Is Exchange Transfusion Necessary?
is necessary when conventional treatments fail to manage blood-related conditions effectively. For instance, in newborns with severe jaundice, high bilirubin levels can lead to brain damage if not treated promptly. Similarly, in sickle cell disease, the procedure helps in reducing the number of sickle-shaped cells, thereby preventing complications like stroke and organ damage.
How Is the Procedure Performed?
The procedure is typically performed in a hospital setting under the supervision of experienced medical professionals. It involves inserting a catheter into a large blood vessel, usually in the arm or groin. Blood is then removed in small amounts and replaced with donor blood or plasma. The process is repeated until a significant portion of the patient’s blood has been exchanged. This meticulous process requires careful monitoring of vital signs and blood parameters to ensure patient safety.
Who Needs Exchange Transfusion?
is recommended for patients with specific medical conditions that cannot be managed with standard treatments. These include:
- Newborns with severe jaundice
- Patients with sickle cell anemia experiencing severe complications
- Individuals with certain types of poisoning or drug overdose
Case Study: Neonatal Jaundice
Consider a newborn diagnosed with severe jaundice. Despite phototherapy, bilirubin levels remain dangerously high. In such cases, an exchange transfusion can rapidly reduce bilirubin levels, preventing potential brain damage. This intervention is crucial in managing acute cases where time is of the essence.
Case Study: Sickle Cell Anemia
In patients with sickle cell anemia, exchange transfusion can be life-saving. For example, a patient experiencing a severe pain crisis or acute chest syndrome may benefit from the procedure. By replacing sickle-shaped cells with normal red blood cells, the risk of complications is significantly reduced.
What Are the Risks and Benefits of Exchange Transfusion?
Like any medical procedure, exchange transfusion comes with its own set of risks and benefits. Understanding these can help patients and caregivers make informed decisions.
Benefits
- Rapid reduction of high bilirubin levels in newborns
- Decreased risk of complications in sickle cell patients
- Effective removal of toxins in cases of poisoning
Risks
- Potential for infection at the catheter site
- Risk of blood clots or bleeding
- Allergic reactions to donor blood
Despite these risks, the benefits of exchange transfusion often outweigh the potential complications, especially in life-threatening situations.
How to Prepare for an Exchange Transfusion?
Preparation for an exchange transfusion involves several steps to ensure the procedure’s success and patient safety. Patients may need to undergo blood tests to determine compatibility with donor blood. Additionally, fasting may be required before the procedure, and patients should inform their healthcare provider of any medications they are taking.
Pre-Procedure Requirements
Before the procedure, patients will undergo a thorough medical evaluation. This includes blood typing and cross-matching to ensure compatibility with donor blood. Patients may also need to fast for a few hours before the procedure to reduce the risk of complications.
Post-Procedure Care
After the exchange transfusion, patients are closely monitored for any adverse reactions. Vital signs are checked regularly, and blood tests are conducted to assess the effectiveness of the procedure. Patients may need to stay in the hospital for observation, depending on their condition and response to the treatment.
Frequently Asked Questions
What is the success rate of exchange transfusion?
Exchange transfusion has a high success rate, especially in treating neonatal jaundice and sickle cell complications. Success depends on the underlying condition and timely intervention.
How long does the procedure take?
The procedure typically takes 2-4 hours, depending on the amount of blood that needs to be exchanged and the patient’s condition.
Are there any alternatives to exchange transfusion?
Alternatives may include phototherapy for jaundice or medication for sickle cell disease. However, exchange transfusion is often the most effective option in severe cases.
Is exchange transfusion safe for newborns?
Yes, when performed by experienced medical professionals, exchange transfusion is safe for newborns and can prevent serious complications.
What should I expect during recovery?
Recovery involves close monitoring in a hospital setting. Patients may experience mild discomfort at the catheter site, but serious complications are rare.
Can adults undergo exchange transfusion?
Yes, adults can undergo exchange transfusion for conditions like sickle cell disease or severe poisoning. The procedure is tailored to the patient’s specific needs.
Contact HealthHop for assistance in booking your medical procedure overseas and start your journey to affordable, world-class healthcare today!